Patient Care
Providing quality care
Emergency medicine is the medical specialty dedicated to the diagnosis and treatment of acute illness and injury. It includes the initial evaluation, diagnosis and treatment of any patient requiring expeditious medical, surgical or psychiatric care.
At the Dalhousie Department of Emergency Medicine, our top patient care priority is improving access to quality care.
Our second major area of focus is improving population outcomes. Our department oversees the provincial trauma program, the poison control centre, and Nova Scotia’s ground and air EMS system. We also contribute to the province-wide Clinical Services Plan in an effort to improve emergency care across Nova Scotia.
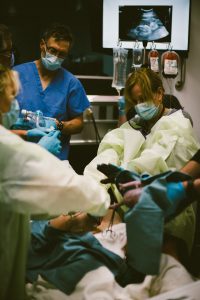
Emergency physicians receive specialized education in the resuscitation and stabilization of critically ill and injured patients. This includes advanced training in airway management and other potentially life-saving procedures. It includes the diagnosis, early recognition and appropriate treatment of the severe complications of disease (from heart attack to stroke, anaphylaxis to meningitis, and trauma to poisoning, etc). And it includes the crisis management skills and experience to lead interdisciplinary teams and remain focused and calm under pressure. Emergency physicians are prepared and capable of responding to the sickest patient in their community that could possibly present to the emergency department at any time.
Emergency physicians also receive a broad education in acute generalist medicine. Significant and serious illness and injury can present in subtle or non-specific ways. Ruling out or making important diagnoses requires a working knowledge of a wide spectrum of physical and mental pathophysiology, and an understanding of how patient symptoms can be embedded in socio-cultural contexts. Cost-effective diagnostic evaluations, evidence-based treatment strategies and values-based patient care are all at the core of the discipline of emergency medicine and fundamental to its patient care mission. Emergency physicians also receive extra training in critical thinking, the art and science of decision making, critical appraisal of the medical literature and diagnostic reasoning.
Emergency medicine (perhaps more so than any other medical or surgical specialty) is not a silo unto itself. The practice of Emergency medicine is inherently multidisciplinary and interdependent upon multiple pre-hospital, in-hospital, and health system-wide structures and processes. Emergency physicians work closely with their nursing and paramedic colleagues in the service of patient care in the emergency department. Emergency physicians are involved in primary, secondary and tertiary prevention strategies, compliment the role of primary care physicians, and collaborate with other specialists and sub-specialists in the continuum of care and return to health. Emergency physicians also contribute to patient care at the population/public policy level through their leadership and design of trauma systems, regional poison control centres, disaster/mass casualty planning and other integrated networks of emergency (cardiac, stroke, sepsis, neonatal, air medical transport, etc, etc) care.
Practically, the type of patient presentations that are considered to be ideally treated in an emergency department run the spectrum from Canadian Triage and Acuity Scale (CTAS) level 1 – the most acute, to CTAS 5; from major trauma (e.g. motor vehicle crash or gunshot wound), to a small child with fever and lethargy (rule out meningitis or other serious infection), to a laceration of the hand (rule out neurovascular or tendon injury). When considered in this way there are important implications that follow with regards to educating physicians, improving inter-disciplinary teamwork, and optimizing system design to improve patient and population outcomes.
Emergency Medicine |
Unforeseen
|
Predictable Scheduable |
|---|---|---|
| CTAS 1, 2 | Critical Care of the acutely ill and injured
|
|
| CTAS 3 | Critical Decision making in undifferentiated/unscheduled health events
|
Potentially “avoidable” ED visits: (ED as safety net)
|
| CTAS 4, 5 | Appropriate ED visits
|
Potentially “inappropriate” ED visits: (ED as gate keeper)
|
To improve patient outcomes for the acutely ill and injured, timely access to high quality and well trained Emergency Physicians and their colleagues in nursing and paramedicine is essential. While system design and staffing models of care should focus on the unscheduled CTAS 1,2,3 patient population, managing unscheduled CTAS 4,5s in the ED improves quality, is cost effective, and does not contribute to ED access block. Preventing ED visits from the complex (frail elderly, chronic dx, no acute medical event), but potentially schedulable patient cohort, would significantly improve ED flow and overall patient care in the ED.
- ACEP definition of Emergency Medicine
- MYTH: Emergency room overcrowding is caused by non-urgent cases – October 2009 Canadian Health Research Foundation Myth Buster of the year series
- The Effect of Low-Complexity Patients on Emergency Department Waiting Times Schull MJ, Kiss A, Szalai JP. Ann Emerg Med. 2007 Mar;49(3):257-64, 264.e1. Acad Emerg
- The Costs of Visits to Emergency Departments, Robert M Williams , M.D., PhD (N Engl J Med 1996;334:642-6.)
- Emergency Medical Care: 3 Myths Debunked, Huffington Post. Leigh Vinocur, M.D. Director of Strategic Initiatives at the University of Maryland School Medicine.
“Please be conscious of the energy you bring into this caring space.
We come here to provide you with the care you need.”
CAEP Position Statements
EMERGENCY MEDICINE CARE
Choosing Wisely CanadaTM Choosing Wisely Nova ScotiaTM and Patient Information
NSHEN Choosing Wisely Fireside Chat with Dr. Connie LeBlanc & Dr. Sam Campbell
We want to provide the right care for all our patients. According to a study conducted by the Canadian Institutes of Health Information (CIHI) as much as 30% of what we to to and for patients in Canada provides no benefit to the patient. As every test and medication carries some risk, we strive to reduce this excess by Choosing more Wisely.
This is a list of tests and treatments that are often of no added value to our patients and we strive to use these science-based guidelines to inform our care.
These patient information pamphlets provide more information on how to make sure your care is the safest possible.
-
- Violence in the Emergency Department- Abusive behaviors towards our staff will not be tolerated in this setting
- Hospital Crowding– In reality the ED is crowded because the hospital is crowded
- ED care for the elderly (PDF – 381 Kb) – Most of our ED physicians have specific training in caring for older patients
- Sick notes (PDF – 558Kb)
RISK MITIGATION
-
- Gun control (PDF – 273 Kb) – Having a gun in your home increases the change of gun death.
- Cell phones and driving (PDF – 156 Kb) – You are 23 times more likely to crash is using your cell phone while driving.
- Bicycle safety (PDF – 185 Kb) – Helmets save and drivers must play their part too.

